Quick Summary
Behavioral Health RCM is the specialized revenue cycle process for mental health and substance use disorder (SUD) treatment programs. It entails extended treatment durations, strict 42 CFR Part 2 consent requirements, multiple-payer rules, and related issues. Mastering it ensures financial stability, reduces A/R days, and allows clinicians to focus on quality care.
Why Listen to Us
At Prosperity Behavioral Health, we partner with detox, residential, PHP, and IOP programs, managing the entire RCM workflow from benefits verification and authorization to claims submission and denial prevention. As the CEO of a Multi-Location Behavioral Health Network shared, we delivered significantly higher collections, fewer denials, and complete visibility into their financial health.

Having processed more than $1 billion in claims annually, our team brings proven insights on improving cash flow and minimizing denial rates for the brands we serve.
Ready to Improve Your Behavioral Health RCM?
Behavioral health providers dedicate themselves to patient healing, yet they are crippled by alarmingly high claim denial rates.
Ongoing prior authorizations, strict time-based coding, and complex documentation requirements for mental health and substance use treatment create endless delays, appeals, and revenue leakage.
Fortunately, you can overcome these obstacles and recover your lost revenue.
This guide defines behavioral health RCM, explores its key differences with general health RCM, breaks down the full revenue cycle step by step, shares benchmarks, and explains when to consider outsourcing to specialized partners.
What is Behavioral Health RCM?
Behavioral health RCM is the financial process that mental health and substance use treatment organizations rely on to manage the entire patient journey, from the first interaction through payment collection.
It covers key steps such as patient registration, service documentation, insurance verification, claims submission, payment posting, and ongoing administrative oversight.
Unlike general health, behavioral health introduces extra layers of complexity. Payer rules differ across session types. Strict prior authorizations are common. Yet, when behavioral RCM operates effectively, through specialized expertise and accurate documentation, the impact is transformative:
- Providers achieve financial stability through accurate reimbursement for vital services such as psychotherapy.
- Clinicians focus on delivering high-quality care without administrative bottlenecks.
- Patients experience a more transparent billing process with clear expectations upfront.
- Staff channel their energy into supporting patients’ healing and fostering long-term recovery.
A well-structured behavioral health RCM system boosts efficiency and cuts claim denials, building lasting financial strength for practices dedicated to mental health care.
Why Behavioral Health RCM is Different from General Health RCM
Behavioral health RCM differs from general health RCM primarily because behavioral health services involve long-term and continuous treatment models focused on mental health and substance use disorders. We will discuss key differences between the duo, including the nature of care delivery, coding and documentation demands, and more.
1. Authorization-Driven Care
Standard procedures in medical settings proceed with minimal prior-authorization friction. Providers’ full focus on clinical delivery with smooth reimbursement pathways.
Behavioral health, by contrast, is more demanding. The services offered, such as individual or group psychotherapy, are subject to rigorous prior authorization requirements. Providers are compelled to submit comprehensive clinical documentation upfront every few weeks or months. This intense scrutiny arises from several payer concerns:
- The high costs of behavioral health treatment.
- The highly individualized nature of the mental health and substance use recovery journey.
- A historical under-coverage of mental health conditions.
Take residential substance use disorder treatment as an example. A single 90-day stay can generate 8–12 separate authorization transactions. The initial approval may be followed by concurrent reviews every 3 to 14 days. Staff track expiration dates, assemble detailed submission packets, and follow up to keep active patients covered.
2. Longer Treatment Durations
Revenue cycle management in traditional health RCM follows an episodic path. A patient might come in for a single surgery or a short hospital stay to address an acute issue, and the billing process wraps up shortly thereafter.
In behavioral health RCM, care involves an ongoing therapeutic relationship. Patients return weekly for therapy sessions that stretch across months or years. One patient can generate dozens or even hundreds of individual claims over time. Each session requires fresh coding, documentation, and regular follow-up.
3. Multiple Players With Unique Rules
Behavioral health centers juggle a mix of players. They can include Medicaid, managed Medicaid plans, commercial insurers, or Employee Assistance Programs (EAPs).
Each payer operates with a strict set of rules. One payer might cover unlimited sessions. Another caps therapy at 20 visits per year.
Some payers demand pre-authorization before the first intake session. Others scrutinize every detail during concurrent reviews, cutting off coverage immediately when the documentation falls short.
This challenge is evident in something as straightforward as an Intensive Outpatient Program (IOP). The same group therapy session could be billed using HCPCS code S9480 for many commercial plans, yet switch to H0015 when the focus is on substance use treatment. Use the wrong code, forget a modifier, or miss a payer-specific preference, and the claim is rejected instantly.
4. Strict Patient Consent Requirements
HIPAA permits covered entities to use and disclose protected health information without patient authorization for treatment, payment, and healthcare operations (TPO). This facilitates routine sharing in standard medical settings to support care coordination, billing, quality improvement, and other operational needs.
Behavioral health, on the other hand, operates under a more protective framework. 42 CFR Part 2 imposes stricter safeguards to shield patients from the stigma, discrimination, and legal risks tied to addiction and recovery.
Before submitting any claim that includes SUD diagnosis codes, providers must have a valid Part 2-compliant consent on file. Without that consent, organizations may have to forgo reimbursement or submit claims under non-SUD codes. This risks inaccurate coding, potential audits, and serious compliance violations, increasing the likelihood of denials.
5. Time-Based Telehealth and Session Billing
While traditional health billing revolves around a quick visit, a procedure, or a test, behavioral health operates on a completely different rhythm. Every minute of therapeutic time matters. Whether it’s an in-person session or a telehealth equivalent, providers have to track the actual time spent delivering care. This creates a specialized billing structure centered on session length:
- 90832 for brief sessions (16–37 minutes)
- 90834 for standard mid-length sessions (around 45 minutes)
- 90837 for full-hour therapeutic engagements
But accurate coding is only half the battle. Every claim must be backed by detailed documentation that answers three questions:
- Why was this intervention medically necessary?
- How does it directly address the patient’s condition?
- What outcomes are we working toward?
Without strong documentation, even perfectly timed sessions can be denied under payer scrutiny.
6. Higher Denial Rates
Behavioral health faces higher pushback from payers at every turn. Roughly 41% of providers report denial rates of 10% or higher.
This is rooted in the nature of behavioral care. Mental health and substance use treatment involves ongoing, recurring services that invite repeated payer reviews and heightened skepticism.
Key triggers include:
- Expired or missing authorizations during long treatment courses.
- Progress notes that fail to demonstrate ongoing medical necessity, have mismatched attendance records, or lack sufficient detail on session duration and focus.
- Absent time-based coding elements.
- Coding missteps, such as incorrect time thresholds or mismatches between diagnoses and codes.
All denied claim demands intensive rework, appeals, and write-offs, creating an outsized administrative burden that general healthcare sidesteps.
The Behavioral Health Revenue Cycle Step by Step
Mastering the behavioral health revenue cycle is the key to building a financially resilient practice. We’ll break it down step by step with tips tailored to the complexities of behavioral health.
1. Intake of Patients
The patient intake process is the gateway to a financially healthy practice, a lighter administrative burden, and better therapeutic outcomes for your patients.
The process begins with a phone call, an appointment booking, or a new patient walking through your door. Your team gathers essential information, including demographics, insurance details, relevant mental health history, and referral sources.
A well-executed intake process ensures:
- Every service is accurate, compliant, and aligned with the patient’s needs.
- A welcoming patient experience from day one.
- Elimination of costly downstream bottlenecks and frustrating rework.
- Clarity on financial responsibility, which removes the stress of surprise bills.
2. Benefits Verification
Patients navigating mental health or substance use challenges lead unpredictable lives. They frequently change jobs, lose coverage, or face sudden insurance lapses. Such instability makes Benefits Verification a valuable step in behavioral health RCM.
Verification teams confirm that coverage remains active and covers the planned services. They look into:
- Remaining session limits.
- Any required prior authorizations.
- Co-pay or coinsurance amounts, deductibles, and whether the provider is in-network.
This sets transparent financial expectations for everyone involved, from the practice to the patient.
For example, a plan can impose annual caps on psychotherapy visits, ranging from 20 to 52 sessions yearly. Exceeding these limits without upfront confirmation or proper authorization results in automatic claim denials.
By verifying benefits and determining exact patient responsibility upfront, practices can avoid these issues and ensure care continues without financial surprises.
3. Prior Authorization for Treatment Services
Before clinicians can initiate Mental health and substance use treatment, they must obtain formal approval from the patient’s insurance payer. Insurers impose these requirements to confirm medical necessity and regulate utilization.
This process, known as utilization review, confirms and documents that a patient meets the payer’s medical-necessity criteria for a specific level of care.
Approval hinges on clinical documentation, supported by standardized assessment tools like the LOCUS (for mental health) or ASAM criteria (for substance use disorders). These tools provide structured frameworks for evaluating patient needs and recommending the appropriate level of care.
4. Service Delivery and Clinical Documentation
Next, clinicians bring their expertise to the patient. They deliver individual therapy, conduct in-depth assessments, or manage medications.
Once the session concludes, attention turns to documentation. Clinicians capture the session duration, observed progress, interventions used, and alignment with the established treatment plan.
Payers rely on that documentation to justify reimbursement, while regulators hold practices accountable to specific regulations and individual payer policies.
Completing the notes on the same day or within 24–72 hours ensures your records are accurate, defensible, and audit-ready.
5. Charge Capture of Billable Services
Providers often race through back-to-back patient sessions. Each one carries the potential for billable time, complexity add-ons, or extended-service codes. Overlooking even one session per week can drain thousands in revenue over the course of a year.
That’s where charge capture comes in.
It ensures all billable services are accurately recorded in the billing system after care is delivered. No missed encounters. No accidental duplicates. No coding slip-ups.
Charge capture revolves around these three steps:
- Entry of charges into the management system soon after the visit. Providers capture the date of service, provider, location, and session start/end times.
- The entered charges are compared against appointment schedules, attendance logs, and progress notes to spot and resolve any discrepancies
- Regular daily or weekly reconciliations are done to verify that charges, notes, authorizations, and eligibility align perfectly.
Everything stays in sync, resulting in fewer downstream claim denials and faster payments.
6. Accurate Medical Coding
The details captured in therapy session notes are translated into standardized alphanumeric codes that insurance payers universally understand and accept. The primary code sets include:
- ICD-10-CM for diagnoses
- CPT codes for procedures
- HCPCS Level II codes when additional specificity is required.
That said, the coding process is a logical sequence designed to minimize errors and maximize accuracy:
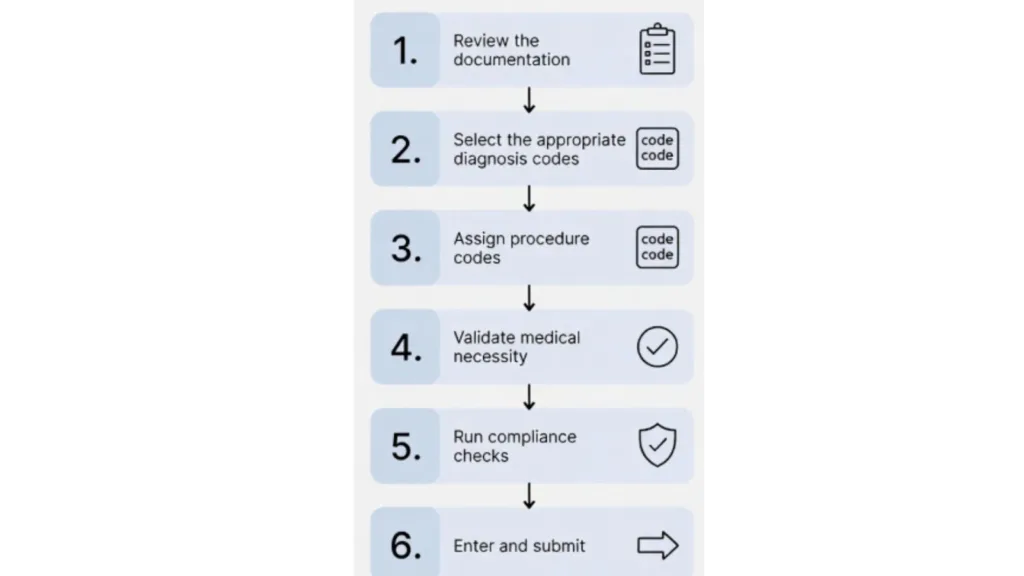
- Review the documentation: Examine progress notes to assess session duration, specific interventions used, and how the service aligns with the respective treatment plan.
- Select the appropriate diagnosis codes: Identify the primary and any secondary ICD-10-CM codes that best capture the patient’s condition and establish medical necessity for the services provided.
- Assign procedure codes: Match the documented services to the correct CPT or HCPCS codes. Pay attention to time thresholds, billable units, and any modifiers needed.
- Validate medical necessity: Ensure each billed procedure is medically necessary and justified by the diagnosis.
- Run compliance checks: Scrutinize the codes against industry regulations to catch potential issues before submission.
- Enter and submit: Input the finalized codes into the system to generate accurate claims for submission.
These processes keep revenue flowing steadily and support both financial sustainability and the uninterrupted delivery of behavioral health care.
7. Claim Submission to Insurance Payers
With your claim fully coded, scrubbed, and perfected, your practice sends it off to the payer for reimbursement. This process is strategic:
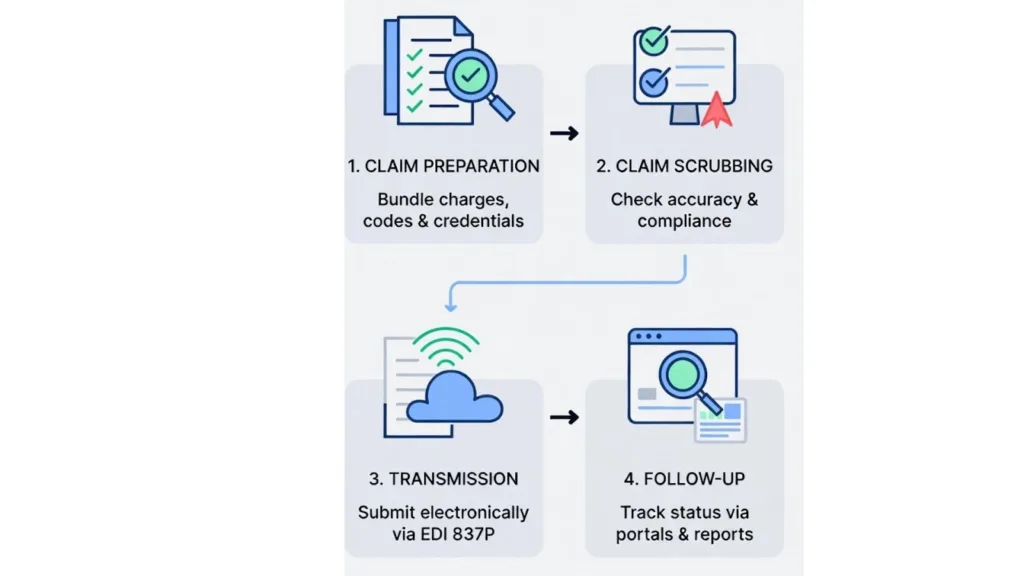
- Claim preparation: Your team bundles charges, CPT/HCPCS codes, provider credentials, and more, ensuring nothing is left to chance.
- Claim scrubbing: Advanced automated tools check submissions for coding accuracy, incomplete data, and compliance with payer-specific rules and flag errors that require rework.
- Transmission: Claims are submitted electronically using the standard EDI 837P format for most outpatient behavioral health services.
- Follow-up: Claim status is tracked via payer portals or clearinghouse reports.
Remember that most payers impose strict windows, commonly 90 to 180 days from the date of service. Build smart calendars, set automated alerts, and treat every deadline like a revenue deadline.
8. Denial Management and Appeals Process
Too many claims come back unpaid due to missing authorizations, incomplete documentation, and other issues. The good news is, a fast response can rescue that lost income instead of writing it off.
That’s where effective denial management comes in.
It’s a structured process that starts the moment payment posting reveals denials, adjustments, or rejections on the remittance advice (RA). It helps spot denied claims, correct what can be fixed, and prevent unfair denials.
Cross-reference the RA with the original claim and supporting documentation. Use Claim Adjustment Reason Codes (CARC) and Remittance Advice Remark Codes (RARC) to categorize each denial, then prioritize high-dollar claims.
For fixable denials, correct the errors and resubmit a clean claim right away. When additional justification is required, attach compelling evidence to strengthen your case.
But if the denial seems unjustified, build your appeal backed by detailed documentation and submit it promptly within 48 hours, and inside the payer’s 30 to 180-day appeal window.
9. Patient Collections and Payment Recovery
Strong collection practices create healthier cash flow that fuels better patient care and a more stable practice.
The key is setting clear expectations from day one. At intake, have transparent financial conversations that explain costs upfront. Collect known copays and deductibles at the point of service, and offer convenient payment options.
Ensure you include flexible plans, online portals, and contactless payments so patients feel supported.
Lastly, conduct timely follow-ups to reduce confusion and minimize bad debt write-offs. Implement automated reminders via text and email that deliver professional, easy-to-understand, itemized statements breaking down the original charges, what insurance covered, and what the patient owes.
Behavioral Health RCM Benchmarks to Track

To stay ahead of cash flow challenges and keep your revenue cycle running smoothly, monitor these behavioral health billing KPIs closely:
- Clean Claim Rate: Aim for 90-95%. A high clean claim rate shows your team is submitting accurate claims the first time, minimizing rework and speeding up payments.
- Days in A/R: Keep this under 45 days. If it starts creeping toward or beyond 60 days, it’s a warning sign of stuck claims or slow-paying insurers, both of which need immediate attention.
- Denial Rate: Target below 5%. This metric shows how often payers reject your submitted claims. Keeping it low means fewer headaches and faster reimbursements.
- Net Collection Rate: Strive for around 95%. This powerful indicator shows how effectively you’re capturing every dollar you’ve earned and reflects the overall health of your billing process.
With the right behavioral health billing KPIs and trend analysis, you gain a comprehensive view of the entire revenue cycle from intake to final payment and catch problems before they drain your practice’s cash flow.
In-House RCM vs. Outsourcing: Knowing When It’s Time to Let Go
While keeping your behavioral health RCM in-house gives you full control over your financial processes, there comes a point when outsourcing becomes the smarter strategic decision.
When billing complexities start eating into your time, delaying payments, and holding back your revenue, it’s a clear signal that change is needed.
By partnering with a specialized RCM provider, you gain access to expert resources and capabilities that are difficult to build and sustain internally.
Signs it’s time to Outsource Behavioral Health RCM
If you’re experiencing any of the following issues, it may be time to consider outsourcing your RCM to a specialized partner who can restore your cash flow:
- AR days are past 45–60. Delayed payments from repeated denials or auth issues might be strangling your cash flow.
- Your net collection rate has dropped below 95%. It’s a sign of revenue leakage caused by unappealed denials, mounting bad debt, or unnecessary write-offs.
- Compliance headaches are piling up. Your internal team is struggling to stay up to date with regulations, putting your practice at risk of audits and penalties.
- Your claim denial rate is above the 5–10% range. Denials might be occurring due to missing authorizations, incorrect CPT codes, improper telehealth modifiers, or other issues.
How Prosperity Behavioral Health Supports Your Behavioral Revenue RCM
Mental health and substance use treatment providers need a partner who understands the complexities of your world.
At Prosperity Behavioral Health, we take full ownership of your entire revenue cycle, from benefits verification and prior authorizations through claim submission, rigorous denial appeals, and collections.
Our exclusive focus on behavioral health means we navigate the coding, payer rules, and utilization review challenges that organizations face every day.
We aim to keep clean claim rates consistently above 95% and days in accounts receivable under 35. That translates into predictable, healthy cash flow so you can confidently expand services, open new locations, onboard more providers, and accept every patient who needs your care. Contact us today if you’re seeking to stabilize your revenue and amplify your mission.

